Children with SRS are at high risk for fasting hypoglycemia because of the combination of their large brain-for-body size, low muscle and liver mass, and feeding difficulties. One study also showed that many of the young SRS subjects had hypoglycemia during the nighttime with no noticeable symptoms. Because ketosis usually occurs before fasting hypoglycemia, SRS specialists recommend the monitoring of urinary ketones as an effective method in the prevention of fasting and/or illness-related hypoglycemia. In addition, SRS children are especially vulnerable during illness or surgery. Intravenous glucose with 10% dextrose may be needed to eliminate ketones and prevent hypoglycemia.
Because hypoglycemia can run the risk of damaging a young, developing brain, we are going to include important preventative information taken from documents created by The MAGIC Foundation as well as excerpted from the book RSS/SRS/SGA – A Comprehensive Guide: Understanding Aspects of Children Diagnosed with Russell-Silver Syndrome or Born Small-for-Gestational-Age, from a chapter titled “Fasting Hypoglycemia and Ketonemia” written by Madeleine D. Harbison, M.D., Richard Stanhope, M.D. and Jennifer Salem, M.A. This information may not be duplicated, copied or plagiarized in any manner.
“Since the concept of ketones is so very important for SRS parents to understand, we shall give a simple and practical overview of a very complex metabolic pathway.
Ketonemia and ketonuria normally precede hypoglycemia. Ketone body formation is associated with both a low blood sugar (hypoglycemia) and a high blood sugar, as in diabetes. In hypoglycemia, there is not enough sugar available to cells and in diabetes, the sugar cannot get into the cells. Normally, cells use sugar, (glucose), as their main fuel. When there is not enough sugar to fuel the cells, they begin to burn fat. Big fat molecules, (triglycerides) must be broken down into smaller molecule to be used as a fuel. Ketone bodies are these smaller, breakdown molecules from fat. The presence of ketones simply means that the cells are getting low on sugar and are using fat as a fuel.
Ketone bodies are weak acids. When they build-up to high levels, they cause a severe acidosis. SRS children may develop a mild acidosis from ketones but never the severe ketoacidosis seen in uncontrolled diabetes. This is because the ketones seen in SRS are associated with a LOW not a HIGH blood sugar.
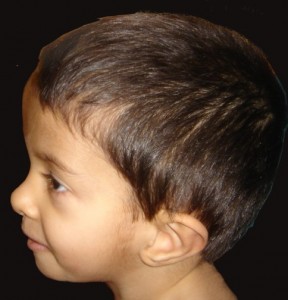
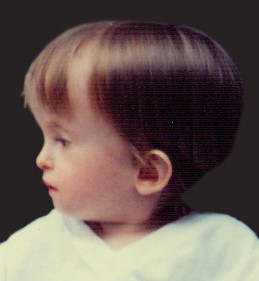
Asymmetric SGA [those with large head-size-for-body] and RSS/SRS children are at an especially high risk of spilling ketones and experiencing fasting hypoglycemia because they have large brains and a small body. BRAIN CELLS cannot use fat as a fuel. The SRS child’s small body can store and make only small amount of sugar. This presents a problem when they do not or cannot eat. Typically, hypoglycemia occurs during physiologic fasting, such as an overnight fast, and during episodes of illness when the child is eating less than usual, is sleeping longer than usual and is requiring more calories because of fever. Unlike the proportionate, normal child who may be able to fast for 8 to 12 hours, the fasting SRS child uses up his stored sugar within 3 to 4 hours. Upon switching to fat as a fuel, ketones appear in the blood and urine and later in the breath. Luckily they can be detected BEFORE the blood sugar drops to a dangerously low level and while the brain still has some glucose to burn. We check for ketones in the urine so that we can detect this switch over to fat burning and thus PREVENT hypoglycemia by giving sugar and complex carbohydrates.**
IMPORTANT: There are some rare, genetic metabolic disorders that prevent normal fat metabolism [SCAD, MCAD and LCAD]. They result in hypoketotic hypoglycemia. This means hypoglycemia without normal production of ketones. For these children, ketonuria does not precede hypoglycemia; thus, monitoring for ketones does not help predict their development of hypoglycemia.
As such, the safest policy is to assume that all SRS children are having nighttime hypoglycemia until proven otherwise, and steps should be taken to prevent hypoglycemia from occurring during the daytime hours. Symptoms are not hard to recognize, both ketonuria and hypoglycemia are easy to test for, and preventative measures are fairly simple to incorporate into the child care routine.
Physical Signs of Hypoglycemia:
- waking to feed at night past early infancy
- excessive sweating
- extreme crankiness improved by feeding
- difficulty waking up in the morning or extreme lethargy when ill and not able to eat
- pallor and shakiness
- poor coordination or odd speech
- ketones in the urine
Testing for Ketones: Parents can easily check for ketones in their child’s urine by using urine ketone sticks or strips that are purchased over-the-counter at a pharmacy. For infants and toddlers who wear diapers, place a couple dry cotton balls in the diaper when the baby urinates. Watch for their wetting and remove the wet cotton ball immediately then squeeze it over the ketone stick or strip. Older children should urinate into a cup and the ketone stick or strip can then be dipped into the urine. The test area’s color will not change if ketones are not present. Otherwise, it will change to a varying hue of purple depending upon the concentration of ketones in the urine. Once this timed reaction is complete, the color of the test area should be compared to the color chart on the side of the bottle. Ketone testing strips and sticks must be kept dry. All ketone measuring methods depend upon the same, moisture-sensitive chemicals in their test areas. Therefore, the strips must be kept tightly capped in a dry area, not a moist bathroom. Purchase a bottle containing the fewest tests; date the bottle when it is opened and use tests from a bottle no longer than one month after opening it. Routine baseline testing of ketones should be done before feeding to determine if the child’s feedings are frequent enough. Typically, the longest period between feeds is overnight. It is best to measure urine ketones after the early morning diaper change. Ketone testing should be done for several consecutive days to be sure that early morning ketones are consistently negative, because of the variability in the amount of food that SRS infants and toddlers eat day to day. If ketones are present in morning urine (or at other times), read the next section on treatment protocols for hypoglycemia and ketonemia.
Testing the Blood Sugar: Talk to your pediatrician or endocrinologist if your child is spilling ketones and/or if you feel your child needs to have his or her blood sugar tested at home. There are many brands of small, hand-held glucose monitoring devices that are ever evolving in their accuracy, ease of use and computer compatibility. There are often coupons on-line for free units, or your physician can write a prescription for a unit and supplies. Also remember, in reality, these meters are made for monitoring diabetics whose blood sugars are more frequently high than low. For this reason, it is important that RSS/SRS/SGA parents make sure that the unit they get is accurate in the lower ranges. Your physician can help facilitate this.
Preventing Hypoglycemia During Nighttime and in Routine Daily Life:
We highly encourage you to read the hypoglycemia chapter in the RSS/SRS/SGA Guidebook for comprehensive prevention and treatment information. However, here are some quick prevention tips:
- feed frequently during the day (sometimes small snacks every 90 minutes helps)
- keep snacks with your child at all times
- avoid juices, sodas or foods high in refined sugar (except when these are needed for a “quick fix” for low blood sugar levels)
- feed through a gastrosomy tube if child cannot maintain blood sugars consistently
- utilize a “snack bag” during school hours to ensure that the child never goes more than 3-4 hours without eating
- use cornstarch or Polycose during nighttime hours (see below)
For SRS infants and children, the nighttime hours of prolonged fasting can represent a high risk period for ketonemia which may progress to hypoglycemia, because both the child and the parents are asleep, making signs of hypoglycemia both harder to spot and frequently unobserved. It is recommended that the parent check the child’s urines for ketone evidence (see prior paragraph) anytime the child’s sleep schedule is extended. For example, if an infant goes from sleeping 4 hours at a stretch to 5 hours, test the baby’s urine with a dry cotton ball at the 5 hour mark. The ketones should be negative for a full week before the parent can assume that it is safe for the baby to fast for this longer period of 5 hours instead of 4 hours. If an infant or child older than 8 months of age spills ketones after a nighttime fast, it is frequently possible to prevent this by adding uncooked cornstarch to his or her last feeding before bed and/or to their middle of the night feed. Giving an individual cornstarch functions like adding to the body’s stores of human starch called glycogen. The body uses the cornstarch for energy first before using the child’s limited glycogen store. An appropriate dose of cornstarch will last for close to 4 hours, and the child’s own glycogen storage will generally add another 2.5 to 4 hours – equaling a total of 6.5-8.0 hours of protection against hypoglycemia. The amount of starch needed to prevent hypoglycemia will depend upon the size of the child and his resting use of calories. Start with one level tablespoon per 4oz of milk or formula and go up as needed. The liquid needs to be stirred or shaken well as the cornstarch can settle. Three flat tablespoons is about the maximum tolerable and suspendable. The cornstarch is tasteless but can be a bit of a texture change – so we recommend slowly introducing cornstarch, beginning by mixing in only 25% of the cornstarch amount, for example, every day for a week. Then gradually increase the amount over time. It is important to remember that below 8 months of age, infants lack the enzyme necessary to break down cornstarch. Younger infants can break down the shorter chains of glucose polymer in the product “Polycose”. Polycose, in its liquid form, may look like light corn syrup but it is not the same. Do not use corn syrup. And never give honey to a child less than 24 months of age. The bottle of Polycose should give dosing recommendations. There are rumors that Polycose may be discontinued so talk to your pediatrician.
Preventing Hypoglycemia During Times of Illness/Vomiting:
If an SRS child is out of sorts and/or seems different from usual, the parents should take the child’s temperature. If the child has a fever, the fever must be treated quickly and efficiently. A fever increases the utilization of calories, and as such, a child may use up his glycogen storage more quickly when experiencing a fever. If an SRS child is unable to eat or hold food down for 4 hours or more, he should be tested for urinary ketones. If he is spilling ketones, the parents stand alerted that their child will progress to hypoglycemia if something does not change. At this point, as early as 4 hours into the illness, the parents must do the following:
- Bring down the fever,
- Give a quick acting dose of carbohydrate such as glucose gel or gel cake decorating frosting,
- Notify the child’s pediatrician,
- Begin testing the child’s blood sugar and
- Attempt a small feed of cool Pedialyte, flat Seven-Up or other soda.
But during bouts of severe gastrointestinal infections (such as rotovirus), the above steps simply may not be enough and the child will need gut rest and an intravenous resuscitation until the child is able to eat normally again.
Many, many parents can attest to the frustration of holding a vomiting child and having an ER doctor say that the child doesn’t need an IV because the child isn’t dehydrated. Ideally, the parent has made prior arrangements with their child’s pediatrician so that standing orders are at the local hospital. But if not, we have written a document that for medical professionals that you can use in times of illness when your child can not eat and needs an IV. We highly recommend that you print out this 2-page document and keep multiple copies in various places such as your car’s glove compartment.
Preventing Hypoglycemia in Surgical/Laboratory Procedures:
As we have said previously, SRS children generally do poorly with fasting of any amount greater than they would on a regular day. Therefore, as a rule of thumb, if a test or an anesthetic procedure requires a child to fast longer than he normally would fast at home, he will need to spend that extra time with an IV in place that delivers glucose. For surgical procedures, this will frequently mean that the child needs to be admitted and have an IV started the evening before surgery. Ideally, an IV solution with 10% solution of glucose plus electrolytes is preferred. Parents must keep in mind that frequently well-meaning surgeons will tell parents, “an IV isn’t necessary because the child is first on the morning’s surgical schedule,” and/or “the procedure is simple and will last only 30 minutes so we do not need an IV”. The reality is that emergencies can come up and a scheduled procedure can be postponed. And although a procedure may only last 30 minutes, afterwards the child may be unable or unwilling to eat so the fasting period is extended. As a result, parents must refuse to budge on this issue.”
In addition, we have a downloadable document to assist you or your physician in the emergency care and treatment of your SRS child. This document was written for families in North America and your physician may have to make adjustments for your country and blood sugar measuring differences.